Copyright © 2007-2018 Russ Dewey
Kubler-Ross
Before the 1970s, psychologists treated death as irrelevant to psychology. Attitudes changed as the result of work by a thanatologist (expert in studying death) named Elizabeth Kubler-Ross. Her book On Death and Dying (1969) was a landmark publication, signaling a new era of open discussion on the topic.
Kubler-Ross got the idea for her book after working with terminally ill patients for two and a half years. In the preface she said her book was not intended as a textbook on how to manage dying patients.
She wanted to "encourage others not to shy away from the 'hopelessly' sick but to get closer to them." Her intention was to encourage loving social contact with the terminally ill. She wrote:
The few who can do this will also discover that it can be a mutually gratifying experience; they will learn much about the functioning of the human mind, the unique human aspects of our existence, and will emerge from the experience enriched and perhaps with fewer anxieties about their own finality. (Kubler-Ross, 1969)
Kubler-Ross identified five stages in the attitudes of a terminally ill patient. These were conceived as interchangeable phases, not necessarily stages in the sense of a fixed sequential ordering of development. In other words, she did not emphasize the exact order of these reactions, just the fact that different, identifiable reactions occurred.
What stages did Kubler-Ross identify?
1. Denial and isolation. The reaction of many people, told they have a terminal illness, is "No, not me! It can't be true! This is a natural defense against the shock of impending death, but usually it is only temporary.
"Among our two hundred terminally ill patients, I have encountered only three who attempted to deny [death] to the very last," wrote Kubler-Ross. The rest moved on to other attitudes.
2. Anger. A distinct phase for many terminally-ill patients was a sense of anger and injustice: "Why me?" This anger emerged at irregular times and was sometimes directed against people who had nothing to do with the basic situation. Often this was a difficult stage for relatives and doctors as well as the patient.
3. Bargaining. Many patients felt they could strike some kind of bargain to postpone death. One type of bargain involved good behavior. Patients stopped smoking, they volunteered to undergo painful therapies, and they devoted themselves to church activities.
Kubler-Ross suggested these patients were operating on the premise that good behavior would be rewarded. If there were justice in the world, death would be postponed or eliminated by sufficient good behavior.
A second sort of bargain involved deadlines, such as a relative's wedding. The patient seemed to say, "God, if you let me live to see this wedding, then you can take me."
Kubler-Ross said patients seldom kept these promises, however. Once the deadline was past, they would set up another deadline or special event to live for, and they would try to prolong the process.
4. Depression. Kubler-Ross wrote, "When the terminally ill patient can no longer deny his illness, when he is forced to undergo more surgery or hospitalization, when he begins to have more symptoms or becomes weaker and thinner, he cannot smile it off anymore." Sometimes patients sink into depression after denial, anger, and bargaining.
5. Acceptance. The final stage of dying is acceptance. It is not a time of joy or happiness but more like "quiet expectation" in Kubler-Ross's words.
Kubler-Ross's five stages have entered popular culture. Discussions of unpleasant events (such as failure of a favored sporting team) might be accompanied by comments like, "People are still in the anger stage..." or "People are entering the acceptance stage..."
Despite Kubler-Ross's explicit statements to the contrary, the 5 stages were interpreted as a series, experienced one after another. This lent itself to satire. On The Simpsons, Homer went through all five Kubler-Ross stages in ten seconds after consuming a deadly blowfish.
What are some criticisms of Kubler-Ross's work?
Critics of Kubler-Ross claimed her scheme could lead to unreasonable pressures on a dying patient. After reading Kubler-Ross, a physician might expect a certain sequence of events.
There were scornful references to a "happy death movement." Critics suggested that patients who did not eventually show acceptance might be seen as difficult or uncooperative.
Kubler-Ross protested that this was a misunderstanding of her work. She never prescribed a proper approach to dying; she just described what she saw. Her recommendations were for compassionate, empathetic, and loving interaction with dying people.
Kubler-Ross also drew criticism when she started dabbling in the occult. She contradicted ideas expressed in the book On Death and Dying suggesting caretakers come to grips with their own finality. A decade later, she started denying that finality.
As Lindsey (1979) reported in The New York Times:
In the past three years...Dr. Ross has begun to encounter growing skepticism from her medical peers over two elements that she added to her theories.
First, she began to offer in her workshops for the dying a strong rope of hope. "There is no death," she said, but "life after life," a happy existence in which all the physical ailments and mental problems of the body disappear.
It was, some critics noted, the same kind of hope that many organized religions offered humanity for ages. This message added considerably to the popularity of her workshops for the dying, according to her aides.
Second, she raised scientific skepticism with her statements that she had encountered "materialized" supernatural spirits. She had given names to four of them–"Mario," "Anka," "Salem," and "Willie."
She said she believed that she had lived in the time of Jesus under the name of Isabel. Dr. Ross has scoffed at the criticism from her peers, saying they would eventually see her as a prophet. (Lindsey, 1979)
Kubler-Ross herself did not have a happy death (Lattin, 1997). She became bitter about the medical establishment and religion.
Kubler-Ross reported bad experiences while hospitalized after a nearly-fatal stroke. She said none of the nurses caring for her, except one, expressed the compassionate attitudes she had worked so hard to recommend.
Hospices existed by the thousands in the U.S., thanks to her work. But (she said) doctors were still reluctant to recommend them to patients. She considered this a defeat. She concluded that her life's work was in vain.
This depressed mental outlook may have been related to the stroke Kubler-Ross suffered. It left her right arm paralyzed and therefore involved her left hemisphere. We saw in Chapter 2 that patients with damaged left hemispheres are more likely to be show depression.
Kubler-Ross might have taken solace from the impact she had on the hospice movement. Using Google's ngram viewer for the word "hospice," one can see that usage of the word went up dramatically right after Kubler-Ross published her book.
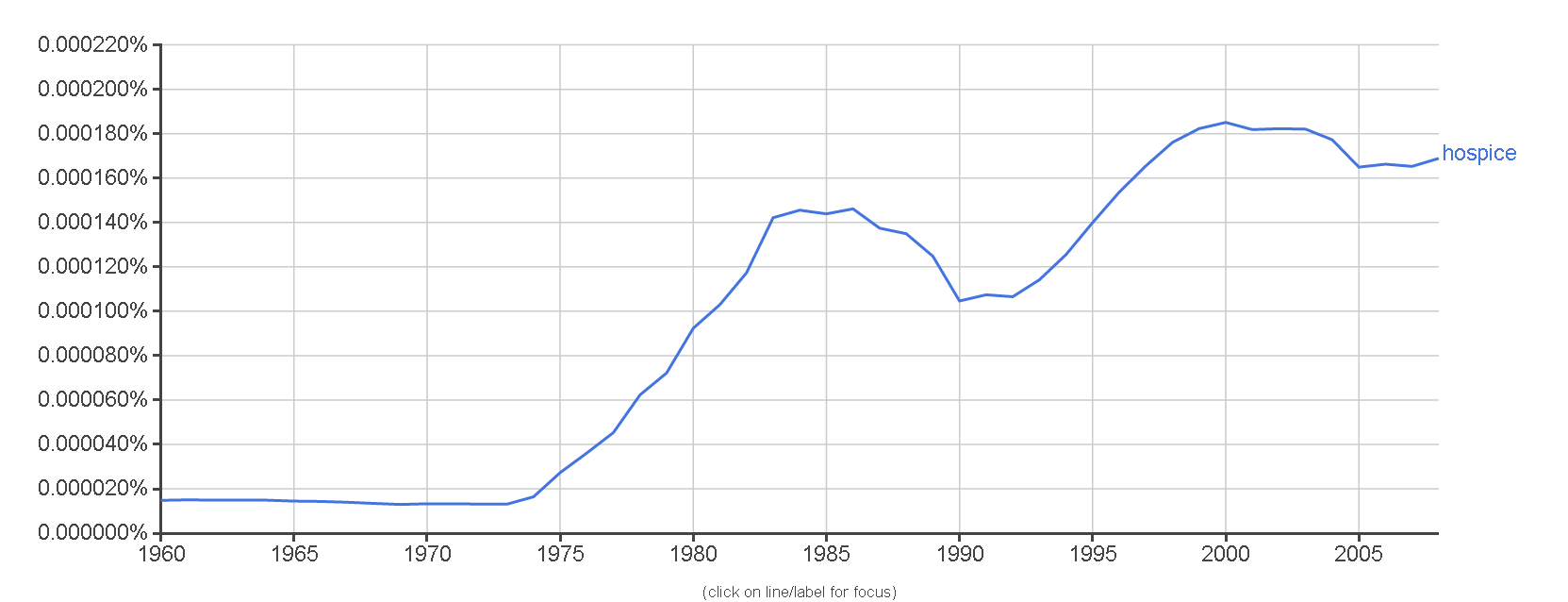
The word "hospice" became used much more frequently after Kubler-Ross's book.
The Hospice Movement
Before the modern era, most deaths from illness took place at home. When a person was seriously ill, there was little to do but keep them comfortable and wait to see if they got better, and that could be done at home.
Then expensive machines became available that could keep dying people alive for months. Such machines are found only in hospitals, so 65% of deaths started taking place in hospitals.
What are some problems associated with hospital deaths?
Sometimes extraordinary measures such as breathing machines only postpone the inevitable. Unless a person fills out a Living Will, asking that extraordinary measures to preserve life not be taken when there is no hope of recovery, doctors feel obliged to use every medical technique available to keep a person alive a little bit longer.
This high-tech approach may destroy the quality of life for a person who only has a few weeks of life left. Instead of lying in bed at home, talking to relatives and sharing memories, a person may spend the last days of life in an intensive care ward of a hospital, hooked to exotic machines or respirators that make conversation difficult.
Such end-of-life extraordinary measures are also very costly, and it is not unusual for an old person's life savings to be consumed in the last weeks of life. About 28% of the Medicare budget goes toward maintaining people in the last year of life, and typical hospital bills for terminally ill patients are between $20,000 and $75,000.
Terminally ill patients who elect not to remain in a hospital setting may decide to spend their last days in hospice care. There is a difference between "a hospice" (a place where terminally ill patients can stay and receive nursing care) and "hospice care" (in which the patient stays at home and receives visits from nurses and other hospice workers).
Hospice care at home is the most common approach in the United States. If a patient has no home or nobody to provide care, a hospice clinic or nursing care facility may be used.
What is the difference between "a hospice" and "hospice care"?
Generally speaking, a patient is admitted to hospice care when a doctor believes the person has less than six months to live and no hope of recovery. That decision can be reversed if a person unexpectedly improves.
While in hospice care, doctors and nurses no longer attempt to fight the disease. All their emphasis is upon palliative care, which means making the patient comfortable.
During hospice care, dosages of painkillers are raised as high as necessary to eliminate pain. Special equipment is provided to make breathing and other basic functions comfortable.
No extraordinary measures are taken to extend life. If a person stops breathing, they are allowed to die. If a person does not want this, they are removed from the hospice care category.
What often happens during hospice care?
One might expect the atmosphere to be sad and depressed during hospice car, but that is seldom the case. In fact, the opposite may be true. Dying patients are often ready to die and happy to spend their last days with loved ones instead of hooked up to machines in a hospital. They typically review life experiences and share valued memories.
Often the most difficult task facing hospice workers is convincing family members to stop pretending the dying person is going to recover. People under hospice care often appreciate honesty and good company more than anything else.
---------------------
References:
Kubler-Ross, E. (1969) On Death and Dying. New York: MacMillan.
Lattin, D. (1997, May 31) Expert on death faces her own death. SFGate. [blog] Retrieved from: https://www.sfgate.com/
Lindsey, R. (1979, September 17). An early leader in counsel for the dying moves into spiritualism. New York Times, p.B10.
Write to Dr. Dewey at psywww@gmail.com.
Don't see what you need? Psych Web has over 1,000 pages, so it may be elsewhere on the site. Do a site-specific Google search using the box below.
